Did you know, around 3,500 men die of prostate cancer every year in Australia, making it the most commonly diagnosed cancer in men nationwide?
About the prostate
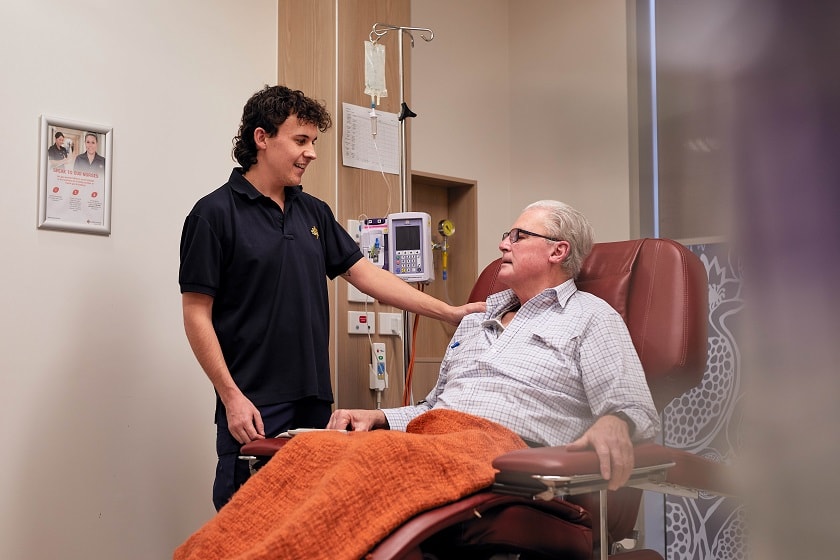
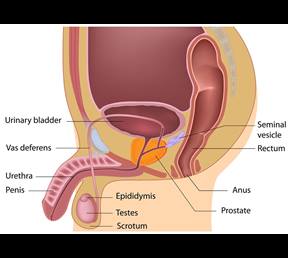
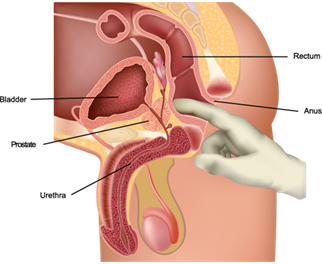
Only found in men, the prostate is a small gland, roughly the size of a walnut, which sits under the bladder and surrounds the urethra (the tube that carries urine and semen through the penis and out of the body). It produces most of the fluid that makes up semen, and needs testosterone to grow and develop.
What is prostate cancer?
Prostate cancer is when abnormal cancer cells grow in the prostate and may spread from the prostate to other parts of the body, especially lymph nodes and bones.
Grades of prostate cancer
Prostate cancer is divided into low, intermediate and high risk categories.
While it’s a slow growing cancer, high risk, or late stage prostate cancer, can grow and spread rapidly compared to the low and intermediate grade prostate cancers, which is why it is important to treat the disease in its early stages.
Symptoms of prostate cancer
The early stages of prostate cancer does not exhibit any symptoms. However, late stage prostate cancer symptoms can include:
- difficulty passing urine (trouble starting or poor urine flow)
- frequent or sudden need to urinate
- discomfort when urinating
- blood in urine or semen
- pain in the lower back, upper thighs or hips.
These symptoms may not mean you have prostate cancer (e.g. a non-cancerous condition of the prostate called Benign Prostatic Hyperplasia can mimic similar symptoms), however, rule of thumb is to see your doctor if you experience any of the above.
Risk factors for prostate cancer
-
Age
The older man gets the greater the chance of getting prostate cancer. For example, the risk of getting prostate cancer by the age of 75 is one in seven men. By the age of 85, this increases to one in five.
-
Family history
Having a first degree relative with prostate cancer increases the risk two or three fold. The risk increases more if there is more than one male relative with prostate cancer.
-
Diet
Some evidence does suggest that a diet high in processed meat, red meat or milk products can increase risk of prostate cancer.
Diagnosis
Examination and blood tests
A doctor will usually do a blood test and/or physical examination to check the health of the prostate.
A physical examination assesses the size, texture and nodularity of the prostate, however, abnormal or normal results don’t necessarily mean you do, or don’t, have prostate cancer.
A blood test may be done to determine the level of Prostate Specific Antigen in the blood. This is a protein produced by the prostate with most of it in semen, and a small amount in the blood. For men with prostate cancer, the level of Prostate Specific Antigen in the blood is higher than normal. However, a high level does not automatically mean that prostate cancer is present. Levels may also be elevated in situations such as:
- prostate infection
- urinary tract infection
- enlargement of prostate
- trauma
- after sexual activity.
Imaging
Scanning the prostate with an MRI machine can detect abnormal areas in the prostate more accurately. This allows more precise targeting of these areas during a biopsy.Prostate biopsy
If tests indicate prostate cancer, you will undergo a biopsy to confirm the diagnosis. This involves taking a small piece of prostate tissue from the abnormal area to be assessed under a microscope. 
Treatment
Treatment of prostate cancer depends on the stage of cancer at the time of diagnosis. If detected early enough, it is termed localised prostate cancer (cancer contained within the prostate).
Localised prostate cancer
This can be treated with:
- Active surveillance: if the cancer is of low volume and low grade, the cancer will be regularly monitored. If the cancer shows signs of progression then definitive treatment is advised.
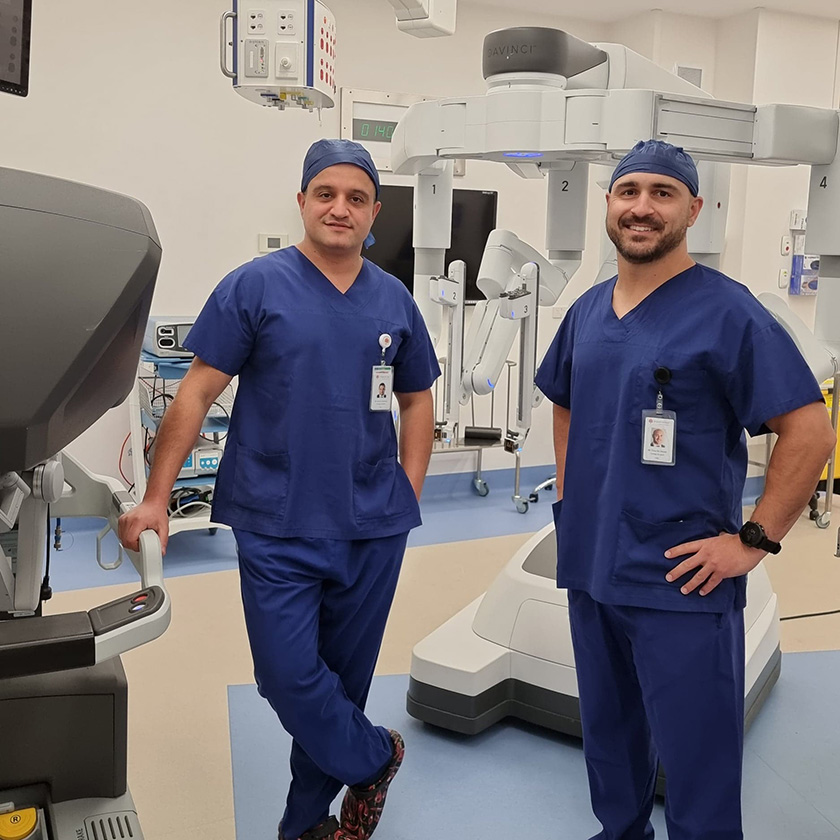
- Radical prostatectomy: this is when the whole prostate is removed. This operation can be done via an open, key-hold (laparoscopic) or robotic approach.
- Radiotherapy: this is where radiation is used to eradicate the cancer cells in the prostate. Patients who opt for this treatment will be referred to a radiation oncologist.
Locally advanced prostate cancer
This is where the cancer has left the confines of the prostate and started to spread to nearby structures. In such situations treatment options are:
- Combined radical prostatectomy and radiotherapy: this is also called multimodal therapy and provides the best chance of cure.
- Radiotherapy alone: in such cases higher doses of radiotherapy are used. Also called high-dose-rate brachytherapy.
Metastatic prostate cancer
Metastatic prostate cancer is when the cancer remains undetected and spreads to other organs, such as lymph nodes and bone. In such cases, a cure is not yet possible, which means treatment turns to slowing the cancer’s growth and controlling symptoms.
If you are concerned, speak to your doctor to seek further information or get tested.
More information
The Prostate Cancer Foundation of Australia has a range of evidence-based sources for men with prostate cancer and their families.
The Prostate Cancer Foundation of Australia also runs support groups around the country that bring together men and women affected by prostate cancer.