- Our services
- Medical and surgical
- Intensive care
Intensive care
Intensive care, also known as critical care, is provided for the sickest patients in hospital.
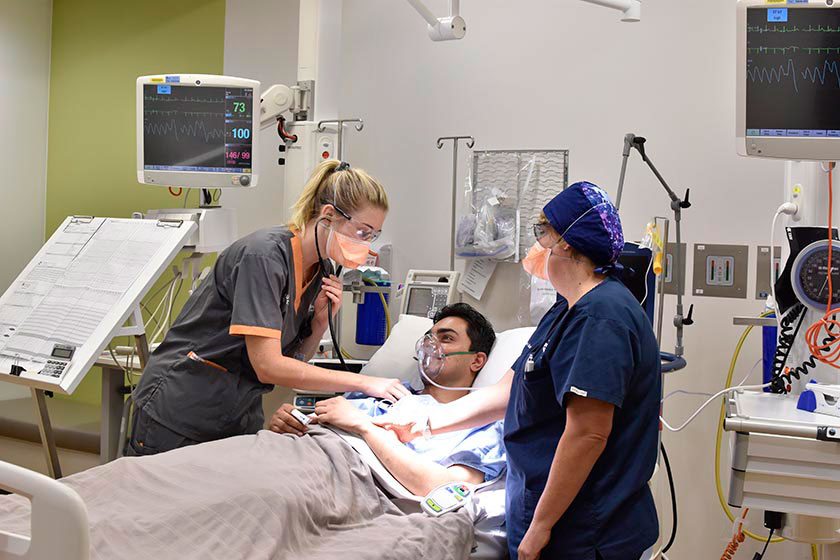
Patients who are admitted to our ICU may need intensive monitoring to protect them from further deterioration, have a life-threatening illness or need treatment for serious injuries after an accident.
Our highly trained intensivists, doctors and critical care registered nurses provide around the clock care, with support from specialist equipment and medications.
Our experienced caregivers provide the best quality of care and liaise with a range of health specialists to provide holistic care for your loved one. We ensure you are kept informed and are included in health care decisions where appropriate.
Our services
Our specialist doctors and nurses have advanced training and experience in providing critical care.
They are supported by state-of-the-art equipment to ensure patients are provided with safe and effective care.
Some of this equipment helps patients to breathe (ventilator), tracks heart activity (heart monitor). Other machines may beep or make other sounds which let our doctors and nurses monitor a patient’s progress and identify if they need urgent attention.
Tubes may also be attached to provide vital fluids or nutrients and remove excess fluids.
ICU caregivers
Patients will receive care from a variety of specially trained staff, they include the following roles:
- ICU doctors: Our specialist intensive care trained consultants and registrars treat and coordinate patient care in the ICU. Throughout a patient’s stay in the ICU, there may be other rostered specialist doctors, such as surgeons, renal specialists, respiratory specialists, and endocrinologist, who will review patients regularly and assist with patient management. If you wish to speak with an ICU doctor about your family member’s care, please enquire about a suitable time to do so with the ward clerk or nursing caregiver.
- Nurses: A range of nurses including Nurse Unit Manager, Clinical Nurse Specialists, Clinical Educators, Clinical Nurses and Registered Nurses are on hand to support the care plan and are available to answer any questions you may have.
-
Pharmacists
-
Physiotherapists: Physiotherapists review patients daily and assist with preventing and managing possible critical care acquired weaknesses. They will commence the rehabilitation process when the patient is stable.
-
Occupational therapists: Occupational therapists can assist patients to manage pressure injuries (ie; bed sores), assess functional task performance to see if specialised equipment can aid their rehabilitation at the hospital or when they return home after being discharged. Our occupational therapists are available to review patients as requested.
-
Dietitians: Often critically ill patients have specific dietary requirements. Our dietitians will ensure that patients receive adequate nutrition based on their individual needs. It is important to check with nursing staff prior to bringing in any outside food or drinks for a patient, as it will need to align with the prescribed diet from our dieticians.
-
Speech pathologists: Speech pathologists are available to review patients as requested. They can assist with swallow and speaking difficulties. They may make recommendations alongside the dietician regarding specific food textures and thickness to prevent accidental choking and chest infection. It is important to check with nursing staff before bringing any outside food or drink to patients.
-
Pastoral Services: Our Pastoral Services team is available to patients, and their visitors, to provide emotional and spiritual support during their hospital stay. The Pastoral Services team forms an integral part of your health care team, providing confidential, professional, pastoral support for people of all backgrounds and beliefs. It is a free service and accessible 24 hours a day. Please speak to one of our caregivers if you would like to speak to a pastoral practitioner.
-
Social workers: Our social workers assist patients and their significant others with the practical, personal and emotional impact of their illness and hospitalisation. They can also provide support or information with accessing community services after a patient is discharged from the hospital.
-
Patient care assistants: Patient care assistants assist nursing staff with patient care and transporting them to and from other department and areas of the hospital.
-
Ward clerks: Ward clerks (administration assistants) provide administrative support for the ICU. They can assist you with directing enquiries, updating contact information and guiding visitors into the unit.
Our Aboriginal Health Team is available for all Aboriginal and Torres Strait Islander patients. The team provides support throughout the patient journey, from time of admission right through to discharge as well as assistance with referral pathways and outpatient appointments, if needed. To contact the Aboriginal Health Team, please speak to a caregiver or contact 9462 4443 or 9462 4436 (business hours only).
Please nominate one main contact person to receive this information either by phone or in person.
Updates only will be given to the nominated person only, as it can be very disruptive to caregivers if they receive multiple calls from varying family members. A family meeting may be initiated by a doctor or it can be arranged by family, to ensure all family members are updated about a patient’s condition.
If you would like to speak to an ICU doctor, please arrange a time via the ward clerk or nursing staff.
Doctors will attempt to speak with you while you are visiting. However, depending on the stability of the other patients, this may not always be practical. The ICU nurse can also provide patient’s updates to family members in person.
Translators are available as required.
Please speak to our nurses to discuss visitor options and restrictions.
Please note that we do not allow visitors into the ICU during handover times.
Doctor’s rounds commence about 9am. They usually start by reviewing the sickest patient first. We appreciate your understanding and patience if you are waiting for your family member to be reviewed by an ICU doctor.
The nurses are allocated to care for up to three patients at a time, depending on the patient’s care needs.
Nursing caregivers attempt to bed wash or shower the patients in the morning. However, this may be delayed if a patient is very unwell. Nursing staff attempt to provide pressure area care every two to four hours to prevent pressure sores (bed sores). You may be asked to wait in the visitor’s lounge while nurses and other caregivers attend to a patient.
Physiotherapists will assist nursing caregivers in getting patients out of bed into chairs or walking in the morning or early afternoon. Chest treatments also will be undertaken for ventilated patients in the morning and afternoon by physiotherapists, as required.
Some patients may require a procedure that is not available at our hospital, such as a coronary angiogram for a patient that has had a heart attack. We will organise such a procedure and the transfer to another hospital, which will be via an ambulance. Once the procedure is completed the patient may return to our hospital if they are stable to do so.
We aim to reduce lights and noise as must as possible in the ICU. However, due to monitors, regular patient checks, and the admission of patients during the night, we recognise the ICU can be disruptive. Patients can ask for eye masks and earplugs to aid in blocking out external stimuli.
The patient will be transferred to an appropriate bed on one of our medical or surgical wards.
The ICU doctors, nurses, and physiotherapists will handover all the required information about the patient’s stay at the ICU to their respective counterparts in the ward the patient is being transferred.
In addition, the ICU Clinical Nurse Specialist will follow up with the patient on the ward the next day, if required, to ensure a smooth transition.
Our research forms part of our focus on continuous improvement and optimising the care we provide to patients.
The ICU team is currently involved in a number of research projects, this includes the design and running of clinical research to improve treatments for a range of conditions, from pneumonia to intensive care acquired muscle weakness. All our research is independently reviewed and ethically approved according to national guidelines.
If you are interested in finding out more or have questions regarding research in the ICU please ask a member of staff.
The Australia and New Zealand Intensive Care Foundation is a not for profit organisation that provides resources to assist patients, family and friends in their journey through ICU and transitioning to the ward.
Resources:
Post-Intensive Care Syndrome (PICS) can occur to anyone after being admitted to the ICU, particularly if they are requiring blood pressure or breathing support. This can result in weakness, delirium and other changes that can be distressing for families and friends to see. The link provides information on the syndrome and how you can assist your loved one through these challenges.
To find out more: Post-intensive Care Syndrome (PICS)
ICUsteps has created an online forum for ICU patients and their families and friends to have access to a community to aid in the understanding of ICU admissions and PICS. Please note that this is for emotional support and sharing experiences only. It does not provide medical advice.
To find out more: ICUsteps | HealthUnlocked
ICU delirium can be distressing for patients experiencing this, as well as for their families and loved ones to witness. To find out more about ICU delirium, what can be expected and tips for assisting someone with delirium, please visit: www.icudelirium.org/
You may be interested in...

